The Body After Breast Cancer, Part 1
Understanding Lymph Nodes, Lymphedema, and the Healing No One Fully Prepares You For
Most people hear the words lymph nodes and immediately feel fear rise in their chest.
I understand that.
In breast cancer conversations, lymph nodes are often mentioned in the same breath as staging, spread, surgery, treatment decisions, and pathology reports. So for many people, the moment lymph nodes come up, the mind goes straight to the worst-case scenario.
But lymph nodes are not the enemy.
They are part of the body’s immune system. They help filter lymph fluid and play a role in helping the body respond to infection, waste, and disease. In breast cancer care, lymph nodes are important because they help doctors understand whether cancer cells appear to have stayed in the breast area or whether they have moved into nearby lymph pathways. The National Cancer Institute explains that a sentinel lymph node is the first lymph node, or sometimes the first group of lymph nodes, where cancer cells are most likely to spread from a primary tumor.
That is why doctors often check lymph nodes in the underarm area during breast cancer surgery.
One of the most common ways this is done is through a sentinel lymph node biopsy. During this procedure, the surgeon identifies and removes the sentinel node or nodes so the pathology lab can examine them for cancer cells. A negative sentinel lymph node biopsy generally suggests the cancer has not spread to nearby lymph nodes or other organs.
Here is the part many people do not realize.
The sentinel lymph node is not always one single node.
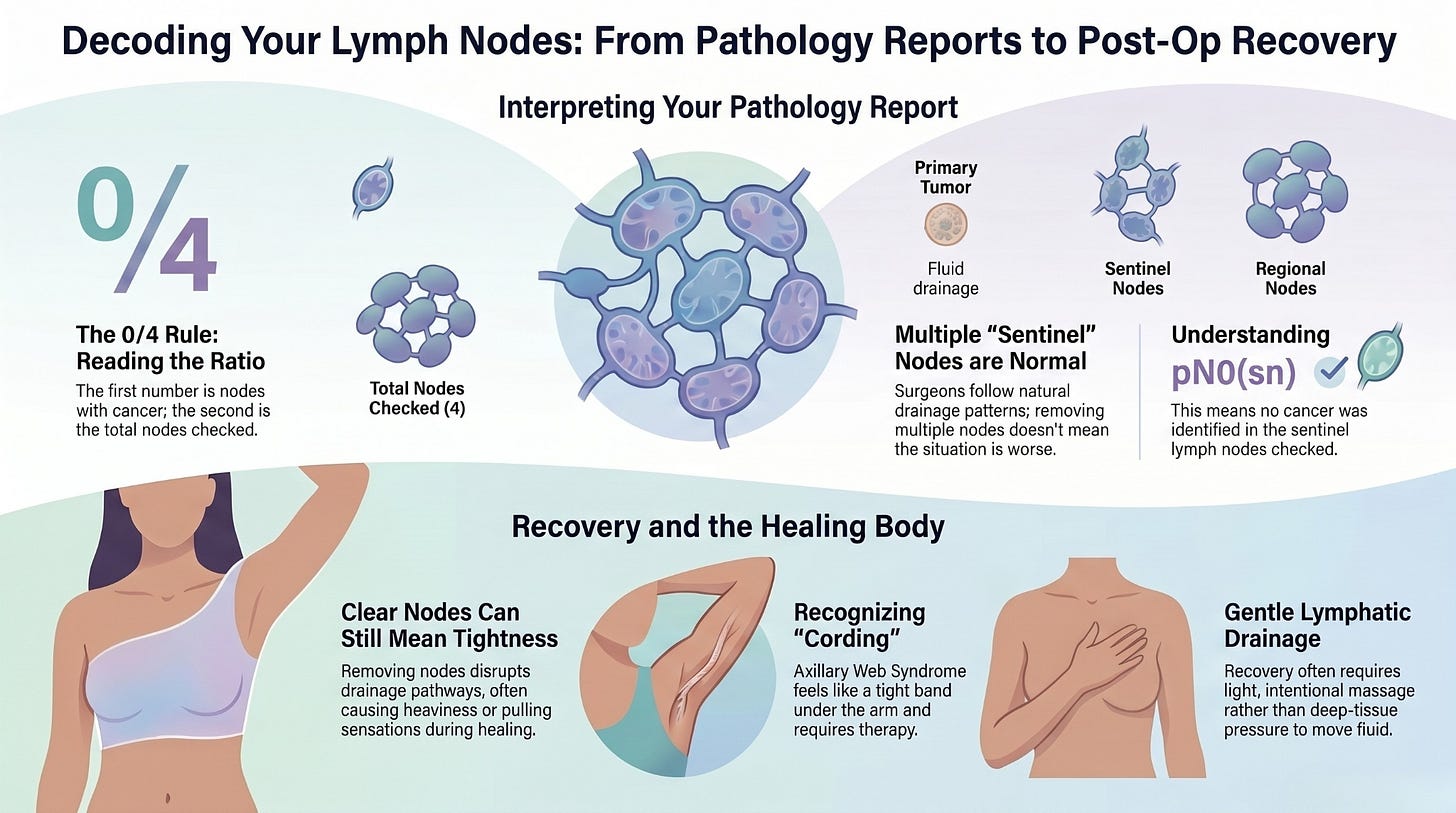
Sometimes there can be more than one sentinel lymph node. That means a pathology report may say one node was removed, or it may say two, three, four, or more were removed. That does not automatically mean the situation was worse. It means the surgeon followed the drainage pattern and removed the nodes that needed to be checked.
This is where reading a pathology report can become confusing.
My own pathology report said:
“Left axillary sentinel lymph node, biopsy: Four lymph nodes, negative for metastasis, 0/4.”
That meant four sentinel lymph nodes were removed from the left underarm area and all four were negative. In plain language, cancer was not found in those four nodes.
That was good news.
My report also listed my lymph node stage as:
pN0(sn)
The “N” refers to lymph nodes. N0 means no regional lymph node metastasis was identified. The sn means the lymph node status was determined through sentinel node biopsy. So in plain English, my sentinel lymph nodes were checked, and they did not show cancer.
But here is what I want more women to understand.
Clear lymph nodes do not always mean the body feels normal afterward.
That is the part we do not talk about enough.
Even when the nodes are negative, the surgery itself can still affect the body. When lymph nodes are removed or damaged during breast cancer treatment, the normal movement of lymph fluid can be disrupted. The American Cancer Society explains that lymphedema can happen when lymph fluid builds up because lymph nodes or vessels have been removed or damaged, and this can lead to swelling, often in the arm or hand after breast cancer treatment.
I know this part personally.
After my double mastectomy, I was diagnosed with lymphedema. I have compression sleeves that I have to wear. I also deal with tightness, especially on my left side, across the breast area, under the arm, and through the area where my body is still healing and rerouting fluid.
That tightness is real.
That heaviness is real.
That feeling of needing to massage the area so fluid can move is real.
And it can feel confusing because you may think, “If my lymph nodes were clear, why am I still dealing with this?”
The answer is that those are two different parts of the story.
Clear lymph nodes speak to cancer status.
Lymphedema and tightness speak to the impact of surgery, lymph fluid movement, scar tissue, healing, and recovery.
One does not cancel out the other.
A person can have negative lymph nodes and still live with lymphedema.
A person can have no lymph node spread and still need physical therapy.
A person can have a good pathology report and still have a body that requires daily attention, support, and care.
The CDC explains that lymphedema can be managed with movement, compression garments, manual lymph drainage, and in some cases pneumatic pumps. Compression sleeves or stockings fit tightly on the swollen arm or leg to help lymph fluid flow out, while manual lymph drainage is a special kind of massage that helps move fluid out of the swollen area.
That is why physical therapy matters so much after breast cancer surgery.
In my case, physical therapy helped me understand that I could not just ignore the tightness. I had to learn how to support my body. I was taught that lymphatic drainage is not deep, aggressive massage. It is gentle, intentional movement that helps encourage lymph fluid to move through the body.
The American Cancer Society also notes that manual lymphatic drainage is a gentle massage technique that can help move lymph fluid out of swollen areas, and a trained therapist may teach someone how to do self manual lymph drainage at home.
That matters because many of us think healing means the incision closed, the drain tubes came out, the surgery was over, and the doctor said things looked good.
But healing after breast cancer surgery can continue long after the visible wound has closed.
There can be tightness.
There can be swelling.
There can be numbness.
There can be pulling.
There can be scar tissue.
There can be fear.
There can be a daily awareness of a body that no longer responds exactly the way it did before.
Some of that tightness may also be connected to something called cording, also known as axillary web syndrome. Cleveland Clinic describes cording as scar tissue that can form under the arm after lymph node removal for breast cancer. It can feel like a tight cord running down the inside of the arm and may cause pain or limit movement. Physical therapy can help improve motion and relieve discomfort.
Again, this is why education matters.
Because when women do not know what they are experiencing, they may suffer in silence. They may think something is wrong with them. They may think they are complaining. They may think they should be “back to normal” by now.
But after a double mastectomy, the body has been through something major.
The lymph system may be adjusting.
The muscles and tissues may be tight.
The nerves may be affected.
The chest wall may feel different.
The arm may swell.
The underarm may pull.
And the person may be trying to process all of this while still showing up for life.
That is why I believe breast cancer awareness has to go beyond pink ribbons and early detection. Those things matter, but awareness also has to include what happens after surgery. It has to include survivorship. It has to include lymphedema. It has to include hormone therapy. It has to include cording. It has to include the daily maintenance many survivors quietly do just to function.
And for hormone receptor-positive breast cancer, treatment may not end with surgery.
Some people are placed on hormone blocker therapy after surgery. Hormone therapy is used for hormone receptor-positive breast cancers because some breast cancer cells use estrogen or progesterone to grow. The American Cancer Society explains that hormone therapy works by either lowering estrogen levels or stopping estrogen from helping breast cancer cells grow.
I am on hormone blocker therapy.
And I want people to understand that this is part of survivorship too.
It is not “just a pill.”
Hormone therapy can come with side effects, body changes, emotional adjustments, and a long-term commitment to reducing recurrence risk. The American Cancer Society notes that hot flashes and night sweats are common side effects of hormone therapy for certain cancers, including breast cancer. Breastcancer.org also lists possible hormone therapy side effects such as hot flashes, vaginal symptoms, loss of libido, fatigue, mood changes, and other medication-specific risks.
That does not mean every person will experience every side effect. It does mean women deserve honest conversations before and during treatment so they can understand what may happen and how to ask for support. I’m experiencing extreme fatigue, weight gain, and joint pain. As stated before, everybody body is different.
This is why understanding the language matters.
A pathology report is not just a medical document. It tells part of the story.
Mine told me that four left sentinel lymph nodes were removed and were negative. It told me the lymph nodes checked did not show metastasis. It told me the cancer was hormone receptor-positive, which helped explain why hormone blocker therapy became part of my treatment plan.
But my body told another part of the story.
My body told me that healing would include tightness.
My body told me that lymphatic care would matter.
My body told me that compression sleeves would become part of my reality.
My body told me that the aftermath of breast cancer is not always visible to other people.
And that is one of the reasons I am becoming more committed to breast cancer awareness and advocacy.
Because there is so much people do not know.
There is so much women are not prepared for.
There is so much we quietly manage after the surgery, after the appointments, after the visible crisis has passed.
Lymph nodes are not automatically bad news.
They are information.
Lymphedema is not a failure of the body.
It is a condition that can happen when the lymph system has been disrupted.
Compression sleeves are not a sign of weakness.
They are support.
Physical therapy is not extra.
For many of us, it is necessary.
Hormone therapy is not simply an afterthought.
For many hormone receptor-positive breast cancer survivors, it is part of the long-term protection plan.
If you are reading your own pathology report or trying to understand your recovery, here are questions worth asking your medical team:
How many lymph nodes were removed?
Were they sentinel lymph nodes?
Were any lymph nodes positive for cancer?
What does my lymph node status mean for my stage and treatment plan?
Am I at risk for lymphedema?
Should I be evaluated by a physical therapist or lymphedema specialist?
Do I need a compression sleeve, and how often should I wear it?
What symptoms should I watch for in my arm, hand, chest, or underarm area?
Could the tightness I feel be cording or scar tissue?
Why was hormone therapy recommended for me, and what side effects should I report?
You are not supposed to automatically know this language.
You are allowed to ask.
You are allowed to say, “Explain that to me in plain English.”
You are allowed to ask again if you still do not understand.
That is not weakness.
That is wisdom.
The more we understand, the less power fear has to fill in the blanks.
And in breast cancer care, those blanks matter. They deserve clarity, compassion, and honest conversation.
This is part one of a series I am calling The Body After Breast Cancer, because surviving breast cancer is not only about what was removed.
It is also about learning how to live in, care for, advocate for, and understand the body that remains.
Educational note: This article is for awareness, education, and support. It is not medical advice. Always discuss your pathology report, symptoms, recovery concerns, and treatment plan with your surgeon, oncologist, physical therapist, lymphedema specialist, or nurse navigator.